Sunday Poster Session
Category: Liver
P1356 - Fatal Fulminant Hepatitis Secondary to Isoniazid Monotherapy for Treatment of Latent Tuberculosis: A Case Report and Literature Review
Sunday, October 27, 2024
3:30 PM - 7:00 PM ET
Location: Exhibit Hall E
- SJ
Sarmand Jameel, MD
Willis Knighton Health System
Shreveport, LA
Presenting Author(s)
Sarmand Jameel, MD1, Shriya Vudari, MD1, Michael Chammany, BS2, Jeffrey Covington, MD3, Veron Browne, MD1
1Willis Knighton Health System, Shreveport, LA; 2VCOM, Shreveport, LA; 3Delta Pathology, Shreveport, LA
Introduction: Latent tuberculosis, represents a dormant phase of tuberculosis that may resurface years later. While individuals with robust immune systems can often harbor Mycobacterium tuberculosis without consequences, a weakened immune system can pave the way for the reactivation of the infection, leading to tuberculosis disease (previously termed active tuberculosis). The standard treatment protocol typically entails nine months of daily isoniazid administration. However, challenges such as hepatotoxicity and the duration of treatment have frequently impeded proper adherence. Although elevations in serum aminotransferase levels are often transient and reversible, there are rare instances where these elevations persist, leading to acute liver injury.
Case Description/Methods: A 56-year-old woman with a complex medical history, including hypertension, diabetes, dyslipidemia, and latent tuberculosis on Isoniazid for the past 3 months, was transferred to our institution for symptoms of nausea, vomiting, and epigastric pain. Upon admission, laboratory tests showed abnormal liver function, an elevated INR, and a positive influenza test. Initial management included antibiotics, Tamiflu, and fluid therapy. Imaging studies revealed fatty liver infiltration The patient's liver function worsened, leading to consultation with the liver transplant service. A liver biopsy confirmed severe liver damage. Despite interventions, the patient's condition deteriorated, leading to altered mental status, hyperammonemia, and renal dysfunction. She was ultimately deemed unsuitable for a liver transplant and died from irreversible liver failure.
Discussion: We present a case of subacute hepatic injury secondary to three months of isoniazid monotherapy treatment for latent tuberculosis infection, culminating in the patient’s death despite discontinuation of all hepatotoxic medications and comprehensive treatment of complications. While cessation of isoniazid has been observed to ameliorate DILI, our case underscores the possibility of irreparable damage persisting beyond cessation of its use. Although the hepatotoxic effects of isoniazid are well-documented, the fatal outcome observed in our case warrants further investigation. The rapid deterioration of our patient despite adherence to guidelines highlights the imperative for enhanced guidance on transplantation timing and optimal management of hepatic injury complications.
Note: The table for this abstract can be viewed in the ePoster Gallery section of the ACG 2024 ePoster Site or in The American Journal of Gastroenterology's abstract supplement issue, both of which will be available starting October 27, 2024.
Disclosures:
Sarmand Jameel, MD1, Shriya Vudari, MD1, Michael Chammany, BS2, Jeffrey Covington, MD3, Veron Browne, MD1. P1356 - Fatal Fulminant Hepatitis Secondary to Isoniazid Monotherapy for Treatment of Latent Tuberculosis: A Case Report and Literature Review, ACG 2024 Annual Scientific Meeting Abstracts. Philadelphia, PA: American College of Gastroenterology.
1Willis Knighton Health System, Shreveport, LA; 2VCOM, Shreveport, LA; 3Delta Pathology, Shreveport, LA
Introduction: Latent tuberculosis, represents a dormant phase of tuberculosis that may resurface years later. While individuals with robust immune systems can often harbor Mycobacterium tuberculosis without consequences, a weakened immune system can pave the way for the reactivation of the infection, leading to tuberculosis disease (previously termed active tuberculosis). The standard treatment protocol typically entails nine months of daily isoniazid administration. However, challenges such as hepatotoxicity and the duration of treatment have frequently impeded proper adherence. Although elevations in serum aminotransferase levels are often transient and reversible, there are rare instances where these elevations persist, leading to acute liver injury.
Case Description/Methods: A 56-year-old woman with a complex medical history, including hypertension, diabetes, dyslipidemia, and latent tuberculosis on Isoniazid for the past 3 months, was transferred to our institution for symptoms of nausea, vomiting, and epigastric pain. Upon admission, laboratory tests showed abnormal liver function, an elevated INR, and a positive influenza test. Initial management included antibiotics, Tamiflu, and fluid therapy. Imaging studies revealed fatty liver infiltration The patient's liver function worsened, leading to consultation with the liver transplant service. A liver biopsy confirmed severe liver damage. Despite interventions, the patient's condition deteriorated, leading to altered mental status, hyperammonemia, and renal dysfunction. She was ultimately deemed unsuitable for a liver transplant and died from irreversible liver failure.
Discussion: We present a case of subacute hepatic injury secondary to three months of isoniazid monotherapy treatment for latent tuberculosis infection, culminating in the patient’s death despite discontinuation of all hepatotoxic medications and comprehensive treatment of complications. While cessation of isoniazid has been observed to ameliorate DILI, our case underscores the possibility of irreparable damage persisting beyond cessation of its use. Although the hepatotoxic effects of isoniazid are well-documented, the fatal outcome observed in our case warrants further investigation. The rapid deterioration of our patient despite adherence to guidelines highlights the imperative for enhanced guidance on transplantation timing and optimal management of hepatic injury complications.

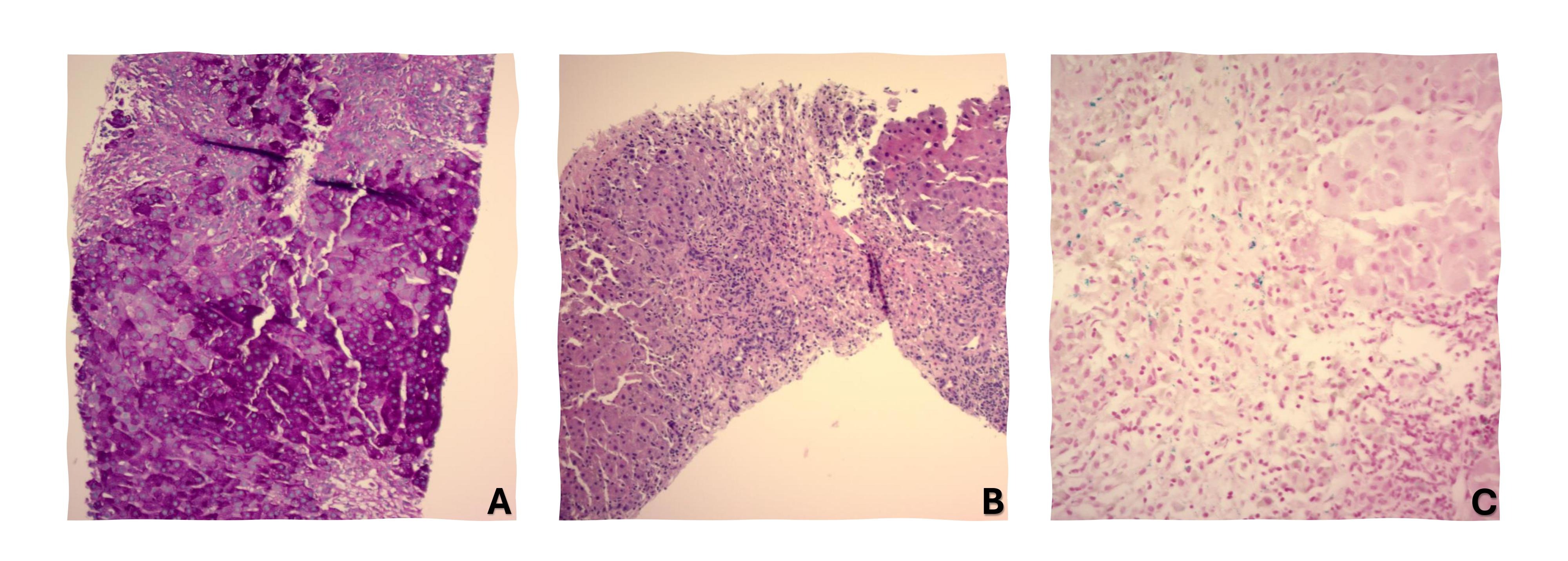
Figure: Figure A: PAS stain taken at 100x showing non-uniform glycogen accumulation in the hepatocytes; common feature in acute hepatitis
Figure B: H&E stain taken at 100x showing areas of residual hepatocytes contrasted next to hepatocyte dropout (necrosis)
Figure C: Iron stain taken at 200x showing some trace accumulation of iron within inflammatory cells; common finding in acute hepatitis or during/after inflammatory insult
Figure B: H&E stain taken at 100x showing areas of residual hepatocytes contrasted next to hepatocyte dropout (necrosis)
Figure C: Iron stain taken at 200x showing some trace accumulation of iron within inflammatory cells; common finding in acute hepatitis or during/after inflammatory insult
Note: The table for this abstract can be viewed in the ePoster Gallery section of the ACG 2024 ePoster Site or in The American Journal of Gastroenterology's abstract supplement issue, both of which will be available starting October 27, 2024.
Disclosures:
Sarmand Jameel indicated no relevant financial relationships.
Shriya Vudari indicated no relevant financial relationships.
Michael Chammany indicated no relevant financial relationships.
Jeffrey Covington indicated no relevant financial relationships.
Veron Browne indicated no relevant financial relationships.
Sarmand Jameel, MD1, Shriya Vudari, MD1, Michael Chammany, BS2, Jeffrey Covington, MD3, Veron Browne, MD1. P1356 - Fatal Fulminant Hepatitis Secondary to Isoniazid Monotherapy for Treatment of Latent Tuberculosis: A Case Report and Literature Review, ACG 2024 Annual Scientific Meeting Abstracts. Philadelphia, PA: American College of Gastroenterology.
